|
12/20/2023 0 Comments Vapotherm high flow nasal cannula 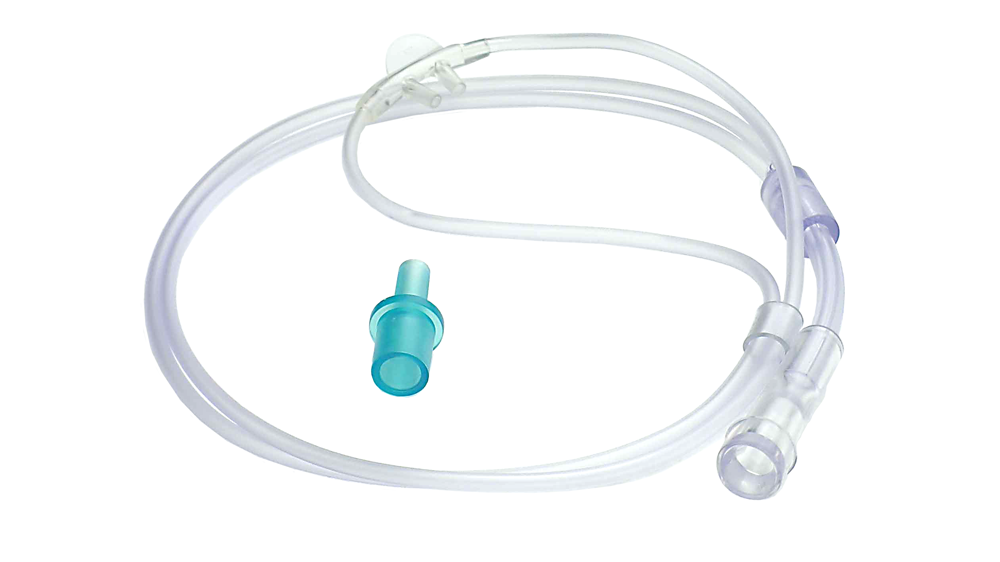
Technological advancements have significantly augmented this concept creating a class of devices called “high flow nasal oxygen.” While there are a variety of HFNO machines available, they can broadly be divided into two groups. Historically, the term 'high-flow' referred to an increased bore size of the nasal cannula with associated gas flow. High flow nasal oxygen (HFNO) is a relatively new modality for treating patients with respiratory failure. Additionally, we discuss studies across clinical settings, including emergency departments, intensive care units, outpatient, and procedural settings. 
In this article, we review the most recent findings on the clinical efficacy of high flow nasal oxygen in Type I, II, III, and IV respiratory failure within adult and pediatric patients. Despite well-described physiologic benefits, the clinical impact of high flow nasal oxygen is still under investigation. High flow nasal oxygen is a relatively new option for treating patients with respiratory failure, which decreases work of breathing, improves tidal volume, and modestly increases positive end expiratory pressure. 4Vapotherm, Inc., Exeter, NH, United States.3Department of Emergency Medicine, University of Tennessee, Chattanooga, TN, United States.2Division of Pulmonary, Critical Care, and Sleep Medicine, Department of Medicine, Icahn School of Medicine at Mount Sinai, New York, NY, United States.1Scientific Consultant, Chattanooga, TN, United States.duPont Hospital for Children in Wilmington, Del., and clinical assistant professor of pediatrics at Jefferson Medical College in Philadelphia.Kara D. Stubblefield is a pediatric hospitalist at Nemours/Alfred I. The mechanics of breathing in children with acute severe croup. The Relationship between High Flow Nasal Cannula Flow Rate and Effort of Breathing in Children. The optimal HFNC rate to decrease effort of breathing for children less than 3 years old is between 1.5 and 2 L/kg/min with the greatest improvement expected in children under 5 kg. The authors did not report the fraction of inspired oxygen settings used, the size of HFNC cannulas, or how PRP changed over several days as HFNC was weaned. There was no difference seen between the two HFNC systems in the study. A rate of 2 L/kg per minute was chosen as a maximum a priori as it was judged the highest level of HFNC patients could tolerate without worsening agitation or air leak. Given the similarity in drop in PRP at 1.5 L/kg per minute and 2 L/kg per minute, the authors suggest this flow rate yields a plateau effect and minimal further improvement would be seen with increasing flow rates. Further examining these younger and lighter patients, the greatest reduction in PRP was in the lightest patients (less than 5 kg). 38), with all significant changes being in patients less than 8 kg ( P less than. When stratifying the subjects by weight, this effect was not statistically significant for patients heavier than 8 kg ( P =. 001) and a slightly smaller but similar reduction in PRP at 1.5 L/kg per minute. Following the trials, patients remained on HFNC as per usual care with twice-daily PRP measurements until weaned off HFNC.Ī dose-dependent relationship existed between flow and change in PRP, with the greatest reduction in PRP at 2 L/kg per minute flow ( P less than. Each patient received HFNC delivered by both systems in sequence with flow rates of 0.5, 1, 1.5, and 2 L/kg per minute to a maximum of 30 L/min. Thirteen patients had bronchiolitis, three had pneumonia, and five had other respiratory illnesses. Prior data suggested a sample size of 20 would be sufficient to identify a clinically significant effect size. Fifty-four patients met inclusion criteria and 21 were enrolled and completed the study. SynopsisĪ single center recruited patients aged 37 weeks corrected gestational age to 3 years who were admitted to the ICU with respiratory distress. SettingĢ4-bed pediatric intensive care unit in a 347-bed urban free-standing children’s hospital. Single-center prospective observational trial. The authors chose systems from Fisher & Paykel and Vapotherm for their testing. 1 An increasing PRP indicates increasing effort of breathing. Placing a manometer in the esophagus allows measurement of the pressure-rate product (PRP), a previously validated measure of effort of breathing computed by multiplying the difference between maximum and minimum esophageal pressures by the respiratory rate. Reliably measuring effort of breathing has proved challenging. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
